Click Here to Download this Blog Post – The Hidden Danger: Why We Look for Vascular EDS (vEDS) (Part 9)
By Dr. Nicholas L. DePace, M..D., F.A.C.C – Cardiologist specializing in autonomic dysfunction, Ehlers-Danlos syndrome and POTS.
When people hear “Ehlers-Danlos Syndrome” (EDS), they usually picture someone who is extremely flexible, double-jointed, or has stretchy skin. While that is true for the most common type (hEDS), there is a much rarer form of the condition that doctors must watch for carefully: Vascular Ehlers-Danlos Syndrome (vEDS).
While the common hypermobile type (hEDS/HSD) can cause pain and fatigue, it is generally considered “benign” regarding life span—meaning patients live a normal length of life.
Vascular Ehlers-Danlos Syndrome (vEDS) is different.
It is a life-threatening condition that affects the body’s internal structures rather than just the joints. Because it carries a high risk of severe complications and a shorter average life expectancy (often into the 40s), diagnosing it early—before an emergency happens—is critical.
It Doesn’t Look Like “Normal” EDS
The trickiest part of diagnosing Vascular EDS is that it breaks the rules of what we think EDS looks like.
- Skin: Unlike the common types, vEDS patients usually do not have stretchy (hyperextensible) skin.
- Joints: These patients are usually not hypermobile in their large joints (like knees or elbows). They might have some flexibility in small joints (like fingers), but they generally don’t pass the “party trick” flexibility tests.
Because they don’t look “bendy,” they often fly under the radar until something goes wrong. This is why heightened awareness is so important.
The Red Flags: Family History and Warning Signs
Since we can’t rely on loose joints to spot vEDS, we have to look at medical history and family history.
If you or a family member have a history of the following, it is a major red flag that requires immediate investigation:
- Unexplained Ruptures: A history of blood vessels bursting or organs rupturing (such as the bowel/intestines) without a clear cause.
- Vascular Dissections: This is when the layers of a blood vessel tear apart.
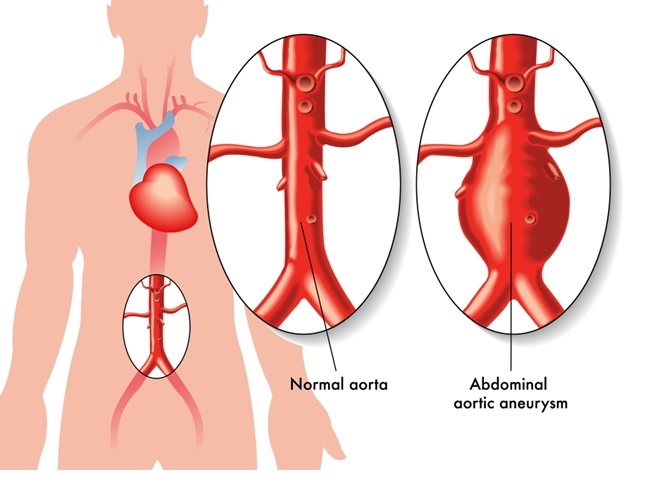
- Aneurysms: Weak spots in arteries that balloon out.
- Severe Bleeding: Bleeding tendencies that go far beyond just “easy bruising.”
- Complications in Childbirth: Abnormal tissue healing or severe complications during labor or gynecological procedures.
Why Vascular Ehlers-Danlos Syndrome (vEDS) Diagnosis Can’t Wait?
With the common hypermobile type of EDS, diagnosis is about managing quality of life. With Vascular EDS, diagnosis is about saving a life.
Knowing a patient has vEDS changes how doctors treat them entirely. It allows us to monitor the blood vessels and take precautions to prevent ruptures. If there is a family history of sudden vascular issues or significant bleeding abnormalities, we do not wait—we test.
It is important to seek out a clinician with expertise in EDS to make an accurate diagnosis and create a treatment plan. One of the nation’s leading centers is Franklin Cardiovascular Associates, under the direction of Nicholas DePace, MD, FACC. They are located in Sicklerville, New Jersey. franklincardiovascular.com, (856) 589-6034
About the Author
Nicholas L. DePace, MD, FACC is a board-certified cardiologist and Medical Director of Franklin Cardiovascular Associates. A graduate of the Mount Sinai School of Medicine, Dr. DePace has decades of clinical, academic, and research experience and has held faculty appointments as a Clinical Professor of Medicine, becoming one of the youngest full professors in Philadelphia at the time of his appointment.
Dr. DePace specializes in the diagnosis and treatment of autonomic nervous system dysfunction (dysautonomia), including POTS, autonomic dysfunction associated with Ehlers-Danlos syndrome (EDS), chronic fatigue, and anxiety-like conditions that are frequently misdiagnosed. He is nationally recognized for his work on parasympathetic and sympathetic (P&S) nervous system imbalance, a core mechanism underlying many complex chronic disorders.
In addition to treating patients from across the United States, Dr. DePace is a prolific clinical researcher and author of multiple nationally distributed medical textbooks published by Springer and W.W. Norton, focusing on autonomic dysfunction, mitochondrial disorders, cardiovascular disease, and mind–body medicine.
👉 View Dr. DePace’s professional profile
👉 View medical books by Dr. DePace